Sean Ninan
@sean9n
Followers
4K
Following
5K
Media
565
Statuses
21K
Actual Geriatrician. LFC. funk, disco, hiphop+onitsuka tigers. tweets about medicine+older people. Also runs a 12 CPD point frailty course @leedsfrailtyed
West Yorkshire
Joined August 2009
@drkateflavs Complaint incoming. Softly spoken Asian lady with bolton accent is actually a formidable litigator. .
19
17
1K
I’m a consultant and I’ve spent large parts of the day in soft play, cooking, and watching David Attenborough documentaries, with some overlap. 4 days a week at work. One day for my boys. No apologies.
I’m a GP. I don’t work Tuesdays. I dropped my kids at school, just had a tennis lesson and I’m meeting my mum shortly to take her to the cinema. All these things keep me sane. No apologies for working “part time”. #teamGP
1
1
102
Two lessons for doctors here 1) not to write off 81 year olds who may have full and active lives and 2) not all fit 81 year olds want to be “for everything.” We should still ask preferences even if we think they should be “for escalation.”.
5
25
96
Positive dipstick does not equal UTI. Positive dipstick does not equal UTI. Positive dipstick does not equal UTI. Positive dipstick does not equal UTI. Positive dipstick does not equal UTI. Positive dipstick does not equal UTI. Positive dipstick does not equal UTI.
Elevated D-dimer does not equal pulmonary embolism. Elevated D-dimer does not equal pulmonary embolism. Elevated D-dimer does not equal pulmonary embolism. Elevated D-dimer does not equal pulmonary embolism.
8
17
93
@DrSdeG @ShaunLintern Like other bad plans, I understood this at the beginning of the pandemic. But not allowing a triple vaccinated, asymptomatic, lateral flow negative visitor wearing the same PPE as I do, to visit their relative with dementia or delirium, seems excessively cruel now.
7
15
85
I find it sad when geriatricians who stop statins due to “limited benefit” think calcium tablets are absolutely essential in the last years of life. What exactly are we trying to achieve?.
Curious witnessing a thread to see 'grown' geriatricians not batting an eyelid over making a nonagenarian with advanced dementia swallow huge calcium tablets. Oh well.
11
11
79
Great to share our trustwide plans for delirium @LeedsHospitals today. Some very important lessons around recognising the person’s capabilities before they came into hospital, the possibility for reversibility, the potential for prevention, and the power of the family/carer
6
21
79
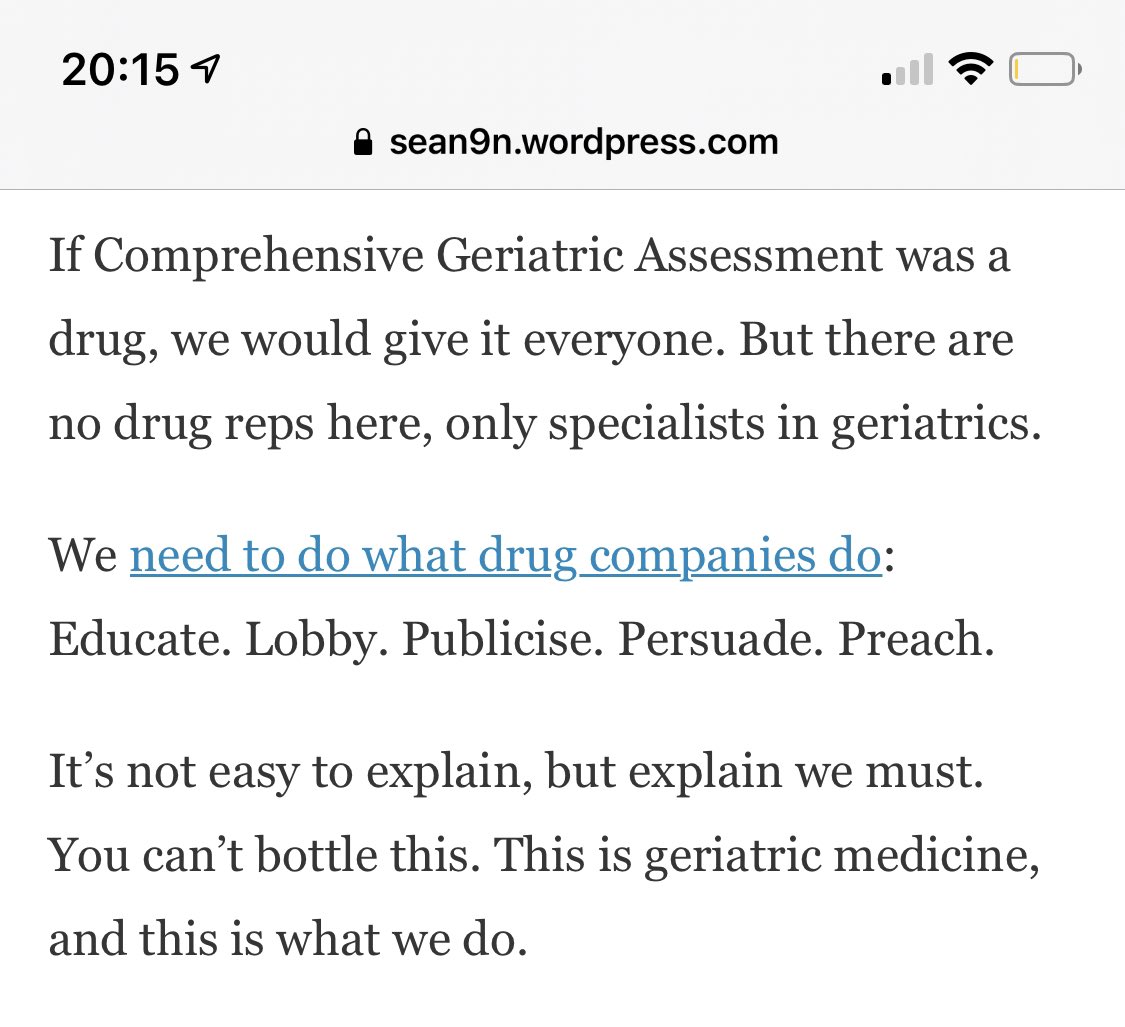
What’s wrong with medicine? A geriatrician’s perspective. @lucypgeridoc @EileenBurns13 @mancunianmedic @Trisha_the_doc @danfurmedge @jupiterhouse1.
9
33
85
Treating older people with frailty is hard. But whether you’re in ED, Acute med, cardiology or general surgery, you need to understand the way to do it. #LeedsFrailtyEducation
0
27
74
85 years old.CFS 3.4AT 12.NEWS 0.A powerful story. If you want to learn more about how useful this concise information is, and how it affects management read my blog and come along to to learn more. @LeedsFrailtyEd.
5
39
67
20-30% of patients in hospital have delirium. Many are missed so we need to sceeen - using a 4AT. prevention is better than cure. We need to systematise good care for patients at risk of delirium. Here’s what to do . @LeedsFrailtyEd.
0
29
61
If you’re a clinician looking after older people in ED or specialty ward? If you’re in primary care doing frailty work but want to learn? If you’re an MDT member doing one part of CGA but wants to find out about the whole? If you’re wondering what the point of CFS, 4AT etc is?👇🏾.
12 CPD points for £80? (virtual) and £120 in person. Too good to turn down! Come and learn about frailty, delirium, dementia, falls, polypharmacy and more in the wonderful city of Leeds.
2
32
52
Why is the NHS less productive? Why are doctors so unhappy? could we fix both these things? With warnings from @ShaunLintern and lessons from @Philippa_Perry @danariely . @Thea_Stein @parthaskar @drohanlon @mgtmccartney @mellojonny.
4
20
51
There are *some* patients who present to hospital with a very clear history of dementia who should just be diagnosed.
Services need to consider how best to identify and diagnose cognitive impairment/dementia at the time of admission for fragility fractures #BGSconf
2
16
53
How many geriatricians think a blood pressure of 120 is “good” for severely frail older people in last couple of years of life? Of course it depends but we are wedded to a model for younger people. “Allow BP 160-170” is something I often write as a manager plan esp if falls.
Older people remain on blood pressure agents despite being hypotensive resulting in increased mortality and hospital admission
7
7
53